132 results
Nutritional composition of ultra-processed plant-based foods in the out-of-home environment: a multi-country survey with plant-based burgers
- R. E. Vellinga, H. L. Rippin, B. G. Gonzales, E. H. M. Temme, C. Farrand, A. Halloran, B. Clough, K. Wickramasinghe, M. Santos, T. Fontes, M. J. Pires, A. C. Nascimento, S. Santiago, H. E. Burt, M. K. Brown, K. H. Jenner, R. Alessandrini, A. M. Marczak, R. Flore, Y. Sun, C. Motta
-
- Journal:
- British Journal of Nutrition , First View
- Published online by Cambridge University Press:
- 15 January 2024, pp. 1-8
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Ultra-processed plant-based foods, such as plant-based burgers, have gained in popularity. Particularly in the out-of-home (OOH) environment, evidence regarding their nutritional profile and environmental sustainability is still evolving. Plant-based burgers available at selected OOH sites were randomly sampled in Amsterdam, Copenhagen, Lisbon and London. Plant-based burgers (patty, bread and condiment) (n 41) were lab analysed for their energy, macronutrients, amino acids and minerals content per 100 g and serving and were compared with reference values. For the plant-based burgers, the median values per 100 g were 234 kcal, 20·8 g carbohydrates, 3·5 g dietary fibre and 12·0 g fat, including 0·08 g TFS and 2·2 g SFA. Protein content was 8·9 g/100 g, with low protein quality according to amino acid composition. Median Na content was 389 mg/100 g, equivalent to 1 g salt. Compared with references, the median serving provided 31% of energy intake based on a 2000 kcal per day and contributed to carbohydrates (17–28%), dietary fibre (42%), protein (40%), total fat (48%), SFA (26%) and Na (54%). One serving provided 15–23% of the reference values for Ca, K and Mg, while higher contributions were found for Zn, Mn, P and Fe (30–67%). The ultra-processed plant-based burgers provide protein, dietary fibre and essential minerals and contain relatively high levels of energy, Na and total fats. The amino acid composition indicated low protein quality. The multifaceted nutritional profile of plant-based burgers highlights the need for manufacturers to implement improvements to better support healthy dietary habits, including reducing energy, Na and total fats.
Proton and helium ions acceleration in near-critical density gas targets by short-pulse Ti:Sa PW-class laser
- Part of
- J.L. Henares, P. Puyuelo-Valdes, C. Salgado-López, J.I. Apiñaniz, P. Bradford, F. Consoli, D. de Luis, M. Ehret, F. Hannachi, R. Hernández-Martín, A. Huber, L. Lancia, M. Mackeviciute, A. Maitrallain, J.-R. Marquès, J.A. Pérez-Hernández, C. Santos, J.J. Santos, V. Stankevic, M. Tarisien, V. Tomkus, L. Volpe, G. Gatti
-
- Journal:
- Journal of Plasma Physics / Volume 89 / Issue 6 / December 2023
- Published online by Cambridge University Press:
- 28 December 2023, 965890601
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
The ability to quickly refresh gas-jet targets without cycling the vacuum chamber makes them a promising candidate for laser-accelerated ion experiments at high repetition rate. Here we present results from the first high repetition rate ion acceleration experiment on the VEGA-3 PW-class laser at CLPU. A near-critical density gas-jet target was produced by forcing a 1000 bar H$_2$
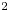 and He gas mix through bespoke supersonic shock nozzles. Proton energies up to 2 MeV were measured in the laser forward direction and 2.2 MeV transversally. He$^{2+}$
and He gas mix through bespoke supersonic shock nozzles. Proton energies up to 2 MeV were measured in the laser forward direction and 2.2 MeV transversally. He$^{2+}$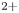 ions up to 5.8 MeV were also measured in the transverse direction. To help maintain a consistent gas density profile over many shots, nozzles were designed to produce a high-density shock at distances larger than 1 mm from the nozzle exit. We outline a procedure for optimizing the laser–gas interaction by translating the nozzle along the laser axis and using different nozzle materials. Several tens of laser interactions were performed with the same nozzle which demonstrates the potential usefulness of gas-jet targets as high repetition rate particle source.
ions up to 5.8 MeV were also measured in the transverse direction. To help maintain a consistent gas density profile over many shots, nozzles were designed to produce a high-density shock at distances larger than 1 mm from the nozzle exit. We outline a procedure for optimizing the laser–gas interaction by translating the nozzle along the laser axis and using different nozzle materials. Several tens of laser interactions were performed with the same nozzle which demonstrates the potential usefulness of gas-jet targets as high repetition rate particle source.
Do we have an “anti-stigmotic”? – Addressing Mental-Illness Related Stigma as the main issue
- C. Cabaços, J. Andrade, F. Pocinho, M. Carneiro, G. Santos, D. Loureiro, A. Macedo
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1031
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
For people with mental illness, internalized stigma, also referred to as self-stigma, is characterized by a subjective perception of devaluation, marginalization, secrecy, shame, and withdrawal. It has many adverse effects on individual’s psychological well-being and clinical outcomes. The iatrogenic effects it has during psychotherapeutic treatment can significantly reduce utilization of mental health care services, reduce quality of life and increase avoidant coping. Overall, internalized stigma is considered a risk factor for poorer mental health prognosis. Although some interventions have recently been developed to specifically intervene on this target as part of psychological recovery goals over the course of treatment, most clinicians are not yet aware or empowered to correctly address this.
ObjectivesDescription of a clinical case illustrating the relevance on addressing internalized mental illness related stigma during the recovery process.
MethodsClinical case report and review of the literature on the subject.
ResultsWe present the case of a 47-year-old female patient, C.S., single, graduated in social work (currently unemployed), who was admitted at the Psychiatry Day Hospital, where she was referred by her Psychiatry Assistant because of abulia, social withdrawal and isolation, depressed mood, thoughts of shame, guilt and self-devaluation and work incapacity. She had been admitted in the Psychiatry ward one year earlier for a first psychotic breakthrough, presenting persecutory and grandiose delusions and auditory hallucinations. After three weeks of inpatient treatment with antipsychotics, a full remission of the symptoms was achieved, without any posterior relapse. Before that first psychotic episode, the patient had been taking anti-depressive medication (escitalopram 20 mg id) for many years, prescribed by her General Practitioner, for mild to moderate depressive symptoms. After being discharged from the Psychiatry ward, C. kept following an outpatient treatment with anti-depressives and behavioural activation-based psychotherapy. She started to believe she was mentally ill and therefore weak, uncapable, and less deserving than her peers or her previous self. These self-stigmatizing ideas were enhanced by the lack of family support and the beliefs that were fostered by her mother, with whom she started to live after the hospitalization. These factors led to a dysfunctional internalization of an illness behaviour, jeopardizing the patient’s ability to reach full recovery.
ConclusionsThis case reinforces the importance of targeting mental illness related stigma during the recovery process. Also, involving the family is of extreme importance to achieve support and address shared beliefs and the interchange between social and internalized stigma.
Disclosure of InterestNone Declared
Neural Abnormalities Associated with Generalized Anxiety Disorder: A Meta-Analysis of Functional Magnetic Resonance Imaging Activation Studies
- S. K. Kahlon, Z. Ali, E. Pritchard, S. Saravia, C. Baten, A. M. Klassen, J. H. Shepherd, G. Zamora, J. Jordan, M. Duran, S. L. Santos, D. W. Hedges, J. P. Hamilton, M. D. Sacchet, C. H. Miller
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S452
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Generalized anxiety disorder (GAD) is a highly prevalent mental illness that is associated with clinically significant distress, functional impairment, and poor emotional regulation. Primary functional magnetic resonance imaging (fMRI) studies of GAD report neural abnormalities in comparison to healthy controls. However, many of these findings in the primary literature are inconsistent, and it is unclear whether they are specific to GAD or shared transdiagnostically across related disorders.
ObjectivesThis meta-analysis seeks to establish the most reliable neural abnormalities observed in individuals with GAD, as reported in the primary fMRI activation literature.
MethodsWe conducted an exhaustive literature search in PubMed to identify primary studies that met our pre-specified inclusion criteria and then extracted relevant data from primary, whole-brain fMRI activation studies of GAD that reported coordinates in Talairach or MNI space. We then used multilevel kernel density analysis (MKDA) with ensemble thresholding to examine the differences between adults with GAD and healthy controls in order to identify brain regions that reached statistical significance across primary studies.
ResultsPatients with GAD showed statistically significant (α=0.05–0.0001; family-wise-error-rate corrected) neural activation in various regions of the cerebral cortex and basal ganglia across a variety of experimental tasks.
ConclusionsThese results inform our understanding of the neural basis of GAD and are interpreted using a frontolimbic model of anxiety as well as specific clinical symptoms of this disorder and its relation to other mood and anxiety disorders. These results also suggest possible novel targets for emerging neurostimulation therapies (e.g., transcranial magnetic stimulation) and may be used to advance our understanding of the effects of current pharmaceutical treatments and ways to improve treatment selection and symptom-targeting for patients diagnosed with GAD.
Disclosure of InterestNone Declared
Major Depressive Disorder Across Development and Course of Illness: A Functional Neuroimaging Meta-Analysis
- C. Baten, A. M. Klassen, J. H. Shepherd, G. Zamora, E. Pritchard, S. Saravia, Z. Ali, J. Jordan, S. K. Kahlon, G. Maly, M. Duran, S. Santos, A. F. Nimarko, D. W. Hedges, P. Hamilton, I. H. Gotlib, M. D. Sacchet, C. H. Miller
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S345-S346
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Functional magnetic resonance imaging (fMRI) has been used to identify the neural activity of both youth and adults diagnosed with major depressive disorder (MDD) in comparison to healthy age-matched controls. Previously reported abnormalities in depressed youth appear to mostly align with those found in depressed adults; however, some of the reported aberrant brain activity in youth has not been consistent with what is observed in adults, and to our knowledge there has not yet been a formal, quantitative comparison of these two groups. In addition, it is not known whether these observed differences between youth and adults with depression are attributable to developmental age or length-of-illness.
ObjectivesThe aim of this study is to elucidate the similarities and differences in patterns of abnormal neural activity between adults and youth diagnosed with MDD and to then determine whether these observed differences are due to either developmental age or length-of-illness.
MethodsWe used multilevel kernel density analysis (MKDA) with ensemble thresholding and triple subtraction to separately determine neural abnormalities throughout the whole brain in primary studies of depressed youth and depressed adults and then directly compare the observed abnormalities between each of those age groups. We then conducted further comparisons between multiple subgroups to control for age and length-of-illness and thereby determine the source of the observed differences between youth and adults with depression.
ResultsAdults and youth diagnosed with MDD demonstrated reliable, differential patterns of abnormal activation in various brain regions throughout the cerebral cortex that are statistically significant (p < .05; FWE-corrected). In addition, several of these brain regions that exhibited differential patterns of neural activation between the two age groups can be reliably attributed to either developmental age or length-of-illness.
ConclusionsThese findings indicate that there are common and disparate patterns of brain activity between youth and adults with MDD, several of which can be reliably attributed to developmental age or length-of-illness. These results expand our understanding of the neural basis of depression across development and course of illness and may be used to inform the development of new, age-specific clinical treatments as well as prevention strategies for this disorder.
Disclosure of InterestNone Declared
Major Depressive Disorder in Youth: A Meta-Analysis of Functional Magnetic Resonance Imaging Studies
- G. Zamora, C. Baten, A. M. Klassen, J. H. Shepherd, E. Pritchard, S. Saravia, Z. Ali, J. Jordan, S. K. Kahlon, G. Maly, M. Duran, S. L. Santos, A. F. Nimarko, D. W. Hedges, J. P. Hamilton, I. H. Gotlib, M. D. Sacchet, C. H. Miller
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S219-S220
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Major depressive disorder (MDD) is a highly prevalent mental illness that frequently originates in early development and is pervasive during adolescence. Despite its high prevalence and early age of onset, our understanding of the potentially unique neural basis of MDD in this age group is still not well understood, and the existing primary literature on the topic includes many new and divergent results. This limited understanding of MDD in youth presents a critical need to further investigate its neural basis in youth and presents an opportunity to also improve clinical treatments that target its neural abnormalities.
ObjectivesThe present study aims to advance our understanding of the neural basis of MDD in youth by identifying abnormal functional activation in various brain regions compared with healthy controls.
MethodsWe conducted a meta-analysis of functional magnetic resonance imaging (fMRI) studies of MDD by using a well-established method, multilevel kernel density analysis (MKDA) with ensemble thresholding, to quantitatively combine all existing whole-brain fMRI studies of MDD in youth compared with healthy controls. This method involves a voxel-wise, whole-brain approach, that compares neural activation of patients with MDD to age-matched healthy controls across variations of task-based conditions, which we subcategorize into affective processing, executive functioning, positive valence, negative valence, and symptom provocation tasks.
ResultsYouth with MDD exhibited statistically significant (p<0.05; FWE-corrected) hyperactivation and hypoactivation in multiple brain regions compared with age-matched healthy controls. These results include significant effects that are stable across various tasks as well as some that appear to depend on task conditions.
ConclusionsThis study strengthens our understanding of the neural basis of MDD in youth and may also be used to help identify possible similarities and differences between youth and adults with depression. It may also help inform the development of new treatment interventions and tools for predicting unique treatment responses in youth with depression.
Disclosure of InterestNone Declared
I don’t know where I’m going or where I come from. Self-disorders in schizophrenia.
- M. D. C. Vallecillo Adame, L. Rodríguez Andrés, C. de Andrés Lobo, T. Jimenez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramirez, M. Fernández Lozano, M. J. Mateos Sexmero, N. Navarro Barriga, B. Rodríguez Rodríguez, M. P. Pando Fernández, M. Calvo Valcárcel, P. Martínez Gimeno, M. A. Andreo Vidal, I. D. L. M. Santos Carrasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1069-S1070
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In the early stages of schizophrenia the person experiences feelings of strangeness about themselves, difficulty in making sense of things and difficulty in interacting with their environment. Based on this, self-disorder assessment instruments have been developed and empirical studies have been conducted to assess people at risk of developing a schizophrenia spectrum disorder. These studies show that self-disorders are found in pre-psychotic stages and that their manifestation can predict the transition to schizophrenia spectrum disorders.
ObjectivesWe present the case of a patient with multiple diagnoses and mainly dissociative symptoms who, after years of evolution, was diagnosed with schizophrenia.
MethodsBibliographic review including the latest articles in Pubmed about self-disorders and schizophrenia.
ResultsWe present the clinical case of a 51-year-old woman with a long history of follow-up in mental health consultations and with multiple hospital admissions to the psychiatric unit, with several diagnoses including: dissociative disorder, histrionic personality disorder, adaptive disorder unspecified psychotic disorder and, finally, schizophrenia. The patient during the first hospital admissions showed a clinical picture of intense anxiety, disorientation and claiming to be a different person. The patient related these episodes to stressors she had experienced, and they improved markedly after a short period of hospital admission. Later, psychotic symptoms appeared in the form of auditory and visual hallucinations and delusional ideation, mainly of harm, so that after several years of follow-up and study in mental health consultations and in the psychiatric day hospital, she was diagnosed with schizophrenia and treatment with antipsychotics was introduced, with a marked clinical improvement being observed.
ConclusionsIt is important to take into account this type of symptoms (self-disorders), as they allow the identification of individuals in the early stages of the disorder and create the opportunity for early therapeutic interventions.
Disclosure of InterestNone Declared
Late diagnosis of attention deficit hyperactivity disorder and cocaine abuse
- C. De Andrés Lobo, C. Vallecillo Adame, T. Jiménez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. Fernández Lozano, N. Navarro Barriga, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Calvo Valcárcel, M. Andreo Vidal, M. P. Pando Fernández, P. Martínez Gimeno, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira, A. Rodríguez Campos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S335-S336
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Adult ADHD diagnosis sometimes represents a challenge for the clinician, due to the comorbid psychiatric diseases that are often associated and which complicate de recognition of the primary symptoms of ADHD. The prevalence of ADHD in adult populations is 2’5% and it is a relevant cause of functional impairment.
ObjectivesPresentation of a clinical case of a male cocaine user diagnosed with adult ADHD.
MethodsLiterature review on adult ADHD and comorbid substance abuse.
ResultsA 43-year-old male who consulted in the Emergency Department due to auditory hallucinosis in the context of an increase in his daily cocaine use. There were not delusional symptoms associated and judgment of reality was preserved. Treatment with olanzapine was started and the patient was referred for consultation. In psychiatry consultations, he did not refer sensory-perceptual alterations anymore, nor appeared any signals to suspect so, and he was willing to abandon cocaine use after a few appointments. He expressed some work concerns, highlighting that in recent months, in the context of a greater workload, he had been given several traffic tickets for “distractions.” His wife explained that he had always been a inattentive person (he forgets important dates or appointments) and impulsive, sometimes interrupting conversations. In the Barkley Adult ADHD Rating Scale he scored 32 points.
He was diagnosed with adult ADHD and treatment with extended-release methylphenidate was started with good tolerance and evolution, with improvement in adaptation to his job and social environment. Since then, the patient has moderately reduced the consumption of drugs, although he continues to use cocaine very sporadically.
ConclusionsEarly detection of ADHD and its comorbidities has the potential to change the course of the disorder and the morbidity that will occur later in adults. Comorbidity in adult ADHD is rather the norm than the exception, and it renders diagnosis more difficult. The most frequent comorbidities are usually mood disorders, substance use disorders, and personality disorders. Treatment of adult ADHD consists mainly of pharmacotherapy supported by behavioral interventions. When ADHD coexists with another disorder, the one that most compromises functionality will be treated first and they can be treated simultaneously. The individual characteristics of each patient must be taken into account to choose the optimal treatment.
Disclosure of InterestNone Declared
The Neural Basis of Major Depressive Disorder in Adults: A Meta-Analysis of Functional Magnetic Resonance Imaging Activation Studies
- A. M. Klassen, C. Baten, J. H. Shepherd, G. Zamora, S. Saravia, E. Pritchard, Z. Ali, J. Jordan, S. K. Kahlon, G. Maly, M. Duran, S. L. Santos, A. F. Nimarko, D. W. Hedges, J. P. Hamilton, I. H. Gotlib, M. D. Sacchet, C. H. Miller
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S158
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Major depressive disorder (MDD) is a highly prevalent mental illness that often first occurs or persists into adulthood and is considered the leading cause of disability and disease burden worldwide. Unfortunately, individuals diagnosed with MDD who seek treatment often experience limited symptom relief and may not achieve long-term remission, which is due in part to our limited understanding of its underlying pathophysiology. Many studies that use task-based functional magnetic resonance imaging (fMRI) have found abnormal activation in brain regions in adults diagnosed with MDD, but those findings are often inconsistent; in addition, previous meta-analyses that quantitatively integrate this large body literature have found conflicting results.
ObjectivesThis meta-analysis aims to advance our understanding of the neural basis of MDD in adults, as measured by fMRI activation studies, and address inconsistencies and discrepancies in the empirical literature.
MethodsWe employed multilevel kernel density analysis (MKDA) with ensemble thresholding, a well-established method for voxel-wise, whole-brain meta-analyses, to conduct a quantitative comparison of all relevant primary fMRI activation studies of adult patients with MDD compared to age-matched healthy controls.
ResultsWe found that adults with MDD exhibited a reliable pattern of statistically significant (p<0.05; FWE-corrected) hyperactivation and hypoactivation in several brain regions compared to age-matched healthy controls across a variety of experimental tasks.
ConclusionsThis study supports previous findings that there is reliable neural basis of MDD that can be detected across heterogenous fMRI studies. These results can be used to inform development of promising treatments for MDD, including protocols for personalized interventions. They also provide the opportunity for additional studies to examine the specificity of these effects among various populations-of-interest, including youth vs. adults with depression as well as other related mood and anxiety disorders.
Disclosure of InterestNone Declared
“The cat and the calcium”. A case of delirium secondary to hypercalcaemia.
- T. Jiménez Aparicio, C. Vallecillo Adame, C. de Andrés Lobo, G. Medina Ojeda, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Fernández Lozano, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, N. Navarro Barriga, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S946-S947
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Interconsultation with the psychiatry service is frequently requested from other specialties for the assessment and treatment of patients who present neuropsychiatric symptoms secondary to organic alterations. On the other hand (and in relation to this case), within the possible causes for the elevation of calcaemia figures, the most frequent are hyperparathyroidism and neoplasms, representing between these two entities 90% of cases (1).
Among the organic mental disorders, Delirium stands out, with an approximate prevalence between 1 and 2% (general population), which increases in hospitalized and elderly patients (2).
ObjectivesPresentation of a clinical case about a patient with delirium secondary to hypercalcemia, with hallucinations and behavioral disturbance.
MethodsBibliographic review including the latest articles in Pubmed about delirium (causes and treatment) and hypercalcaemia secondary to neoplasms.
ResultsWe present a 52-year-old male patient, who went to the emergency room accompanied by his wife, due to behavioral alteration. Two days before, he had been evaluated by Neurology, after a first epileptic crisis (with no previous history) that resolved spontaneously. At that time, it was decided not to start antiepileptic treatment.
The patient reported that he had left his house at midnight, looking for a cat. As he explained, this cat had appeared in his house and had left his entire bed full of insects. His wife denied that this had really happened, and when she told the patient to go to the emergency room, he had become very upset.
As background, the patient used to consume alcohol regularly, so the first hypothesis was that this was a withdrawal syndrome. However, although the consumption was daily, in recent months it was not very high, and at that time no other symptoms compatible with alcohol withdrawal were observed (tremor, tachycardia, sweating, hypertension…).
We requested a general blood test and a brain scan. The only relevant finding was hypercalcaemia 12.9mg/dL (which could also be the origin of the previous seizure). It was decided to start treatment with Diazepam and Tiapride in the emergency room, with serum perfusion, and keep under observation. After several hours, the patient felt better, the hallucinations disappeared, and calcium had dropped to 10.2mg/dL. A preferential consultation was scheduled, due to suspicion that the hypercalcaemia could be secondary to a tumor process.
Image:
 Conclusions
ConclusionsIt is important to rule out an organic alteration in those patients who present acute psychiatric symptoms. Hypercalcaemia is frequently associated with tumor processes (1) due to secretion of PTH-like peptide (4), so a complete study should be carried out in these cases.
Delirium has a prevalence between 1 and 2% in the general population (2).
Psychopharmacological treatment is used symptomatically, with antipsychotics (3). For the episode to fully resolve, the underlying cause must be treated.
Disclosure of InterestNone Declared
Neonatal mortality of lambs in production systems in a semi-arid environment: main risk factors
- J. D. C. dos Santos, E. P. Saraiva, E. C. Pimenta Filho, G. C. X. Neta, L. K. C. Morais, H. S. Teti, S. S. Fidelis
-
- Journal:
- The Journal of Agricultural Science / Volume 161 / Issue 3 / June 2023
- Published online by Cambridge University Press:
- 24 May 2023, pp. 438-449
-
- Article
-
- You have access Access
- HTML
- Export citation
-
The sheep farming has economic and sociocultural importance in semi-arid regions worldwide. Of the total of 1.2 billion sheep in the world, 0.4 are found in semi-arid regions. In this review, we have discussed the main risk factors for neonatal lamb mortality and its association with the prevailing environmental conditions of tropical semi-arid regions. Over the last decades, the average mortality rate of newborn lambs remained relatively constant (~15%) around the world. This rate is reported to be higher (Up to 30%) in small-scale sheep farming systems from developing countries. Overall, the main risk factors of neonatal mortality include low birth weight, dystocia, adverse weather conditions, inadequate milk, or colostrum supply, competition between siblings in multiple births, and poor expression of maternal behaviour. In tropical semi-arid regions, recent findings revealed that newborn lambs from hair coat sheep breeds are less vigorous to perform the first suckling when even exposed to moderate cold conditions (18–20°C). On the other hand, the high radiant heat load in these areas can also challenge the thermoregulation of ewes and newborn lambs, especially if they are kept in areas without protection against direct short-wave solar radiation. Under such circumstances, newborn lambs were reported to be hyperthermic. The heat stress as risk factor for neonatal lamb mortality is a topic that deserves more investigation, particularly in tropical semi-arid areas, where is expected to be drier and hotter as consequence of rapid advances in climate change.
Tobacco use in first-episode psychosis, a multinational EU-GEI study
- T. Sánchez-Gutiérrez, E. Rodríguez-Toscano, L. Roldán, L. Ferraro, M. Parellada, A. Calvo, G. López, M. Rapado-Castro, D. La Barbera, C. La Cascia, G. Tripoli, M. Di Forti, R. M. Murray, D. Quattrone, C. Morgan, J. van Os, P. García-Portilla, S. Al-Halabí, J. Bobes, L. de Haan, M. Bernardo, J. L. Santos, J. Sanjuán, M. Arrojo, A. Ferchiou, A. Szoke, B. P. Rutten, S. Stilo, G. D'Andrea, I. Tarricone, EU-GEI WP2 Group, C. M. Díaz-Caneja, C. Arango
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 15 / November 2023
- Published online by Cambridge University Press:
- 26 April 2023, pp. 7265-7276
-
- Article
- Export citation
-
Background
Tobacco is a highly prevalent substance of abuse in patients with psychosis. Previous studies have reported an association between tobacco use and schizophrenia. The aim of this study was to analyze the relationship between tobacco use and first-episode psychosis (FEP), age at onset of psychosis, and specific diagnosis of psychosis.
MethodsThe sample consisted of 1105 FEP patients and 1355 controls from the European Network of National Schizophrenia Networks Studying Gene–Environment Interactions (EU-GEI) study. We assessed substance use with the Tobacco and Alcohol Questionnaire and performed a series of regression analyses using case-control status, age of onset of psychosis, and diagnosis as outcomes and tobacco use and frequency of tobacco use as predictors. Analyses were adjusted for sociodemographic characteristics, alcohol, and cannabis use.
ResultsAfter controlling for cannabis use, FEP patients were 2.6 times more likely to use tobacco [p ⩽ 0.001; adjusted odds ratio (AOR) 2.6; 95% confidence interval (CI) [2.1–3.2]] and 1.7 times more likely to smoke 20 or more cigarettes a day (p = 0.003; AOR 1.7; 95% CI [1.2–2.4]) than controls. Tobacco use was associated with an earlier age at psychosis onset (β = −2.3; p ⩽ 0.001; 95% CI [−3.7 to −0.9]) and was 1.3 times more frequent in FEP patients with a diagnosis of schizophrenia than in other diagnoses of psychosis (AOR 1.3; 95% CI [1.0–1.8]); however, these results were no longer significant after controlling for cannabis use.
ConclusionsTobacco and heavy-tobacco use are associated with increased odds of FEP. These findings further support the relevance of tobacco prevention in young populations.
Genotype–environment interaction and sexual dimorphism in the genetic evaluation of yearling weight in Simmental cattle raised in Brazil
- G. F. Moura, C.D.S. Arce, J. C. G. Santos, D.J.A. Santos, R. R. Aspilcueta-Borquis, N. T. Pegolo, A. P. C. Gomide, L. F. A. Marques, H. N. Oliveira, F. R. Araujo Neto
-
- Journal:
- The Journal of Agricultural Science / Volume 161 / Issue 1 / January 2023
- Published online by Cambridge University Press:
- 27 January 2023, pp. 148-156
-
- Article
- Export citation
-
The aim of this study was to evaluate the effect of genotype–environment interaction (GEI) on the yearling weight of Simmental cattle raised in Brazil, including the sex dimorphism in reaction norm models. The environmental gradient (EG) was formed using the average weight at 365 days of the contemporary groups. Two approaches were adopted in this study to evaluate reaction norms for weight at 365 days: a single-trait model and a multitrait model in which the data for males and females were separated and considered different traits for the analysis of sexual dimorphism. The genetic parameters were estimated using the Bayesian inference and Gibbs sampling. Analysis of the trend of the heritability estimates obtained with the single-trait model along the EG revealed a value of about 0.33 (EG: −21) in the worst environments, which decreased in the intermediate environments and reached a value of 0.24 in EG: −8, with a subsequent increase of the estimates up to 0.51 in EG: +23. Using the multitrait model, similar trends were observed for the heritability estimates, which ranged from 0.25 to 0.54 for males and from 0.23 to 0.50 for females. The results show that the weight of Simmental cattle raised in the tropics is influenced by GEI and greater genetic progress could be obtained by selecting better environments. However, no significant differences in the response to most environmental changes were observed between sexes and there is only evidence of genetic heteroscedasticity in environments with lower production levels.
My stomach is full
- M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, N. De Uribe Viloria, G. Guerra Valera, T. Jiménez Aparicio, C. Vallecillo Adame, C. De Andrés Lobo, I. Santos Carrasco, J. Gonçalves Cerejeira, N. Navarro Barriga, M.J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Fernández Lozano
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S583
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Anorexia nervosa is an eating behavior disorder that is often related to various personality factors. The relationship between obsessive compulsive disorder and eating Disorders has been highlighted.
ObjectivesTo present a clinical case of a patient with eating disorder and gastric bezoar, secondary to compulsive hair ingestion.
MethodsBibliographic review of articles published in relation to the comorbidity of these disorders, based on articles published in the last 5 years in Pubmed.
Results26-year-old female. Diagnosis of restrictive anorexia nervosa. She was admitted to the hospital on two occasions for nutritional disorders. In the last admission, she reported greater anxiety and significant weight loss. She reports that she has limited her food intake, but she does feel thin and is unable to eat for fear of gaining weight. Ruminative thoughts about her body image. During admission, the patient expressed a sensation of fullness, nausea and vomiting, later observing in abdominal X-ray and gastroscopy, the presence of a gastric trichobezoar, which was finally resolved conservatively.
ConclusionsTrichotillomania is observerd in 1 in 2000 people, trichophagia is even less frequent. According to DSM- V, these disorders are grouped within obsessive-compulsive spectrum disorders. A Trichobezoar is a conglomerate that can be found in the stomach or intestine, composed mainly of hair, previously ingested. Trichotillomania can be associated with anorexia nervosa, especially in patients with obsessive personality traits, which occurs frequently. The gastric slowing that patients with anorexia often present is a factor that favors the formation of the bezoar
DisclosureNo significant relationships.
Alcohol abuse among women: a review with a gender perspective
- J. Gonçalves Cerejeira, I. Santos Carrasco, C. Vallecillo Adame, C. De Andrés Lobo, T. Jiménez Aparicio, M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, G. Guerra Valera
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S820
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The harmful use of alcohol is an important risk factor for the health of the population around the world. The incidence of alcohol dependence in women is increasing and both its consumption pattern and its consequences have unique characteristics.
ObjectivesTo present a literature review focused on alcohol use disorder with a gender perspective.
MethodsLiterature review.
Results- Women use to start using alcohol sooner than men and this seems to be a risk factor to become addicted. - Due to physiological and psychological factors women experience more negative health effects from excessive alcohol use than men and it occurs at lower levels of use. - Psychiatric comorbidity associated with alcohol abuse such as anxiety and depression is more common in women and this in turn worsens the alcohol use disorder. - Alcohol consumption increases the vulnerability of women on several levels, including an increased risk of physical abuse.
ConclusionsAlcohol abuse among women deserves special attention and a specific intervention focused on the gender perspective.
DisclosureNo significant relationships.
Something inside my head
- T. Jiménez Aparicio, G. Medina Ojeda, C. De Andrés Lobo, C. Vallecillo Adame, J. Gonçalves Cerejeira, I. Santos Carrasco, G. Guerra Valera, A. Gonzaga Ramírez, M. Queipo De Llano De La Viuda, N. Navarro Barriga, M. Fernández Lozano, B. Rodríguez Rodríguez, M.J. Mateos Sexmero, N. De Uribe Viloria
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S740
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Electroconvulsive therapy (ECT) is a medical treatment for those patients with high suicide risk or refractory psychiatric disorders. It is currently a safe technique, and its effectiveness has been widely demonstrated.
ObjectivesPresentation of a clinical case about a patient with drug-resistant delusional disorder and high suicide risk, who eventually received ECT treatment.
MethodsBibliographic review including the latest articles in Pubmed about ECT procedure, effects and use.
ResultsWe present a 45-year-old man, who visited different doctors several times by reporting he had the feeling of “having a brain tumor or a vascular disorder”, so he requested imaging tests (computed tomography and magnetic resonance). These tests were absolutely normal, but he kept thinking something was wrong, and eventually attempted suicide by hanging (his family founded him before it was too late). The patient was admitted to hospital, and started psychopharmacological treatment, with minimal response. He desperately insisted that he had “something inside his head”. At this point, it was proposed to start ECT, and the patient accepted. After 6 bilateral ECT sessions, he was visibly more relaxed and less worried, and he no longer presented autolytic ideation. He was still a little bit suspicious about the feeling of having a neurological disease. Currently, the patient runs a follow-up consultation.
ConclusionsElectroconvulsive therapy is a safe and effective technique for those patients with high suicide risk. It may be useful to perform imaging tests in certain cases, for detecting intracranial pressure, acute hemorrhage, tumors… A follow-up of these patients must be performed
DisclosureNo significant relationships.
Mutism. What to expect?
- I. Santos Carrasco, J. Gonçalves Cerejeira, M. Fernández Lozano, A. Gonzaga Ramírez, M. Queipo De Llano De La Viuda, G. Guerra Valera, C. Vallecillo Adame, C. De Andrés Lobo, T. Jiménez Aparicio, B. Rodríguez Rodríguez, N. Navarro Barriga, M.J. Mateos Sexmero, E. Pérez, L. Gallardo Borge
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S588
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mutism is the inability or unwillingness to speak, resulting in an absence or marked paucity of verbal output. Mutism is a common manifestation of psychiatric, neurological, and drug-related illnesses. Psychiatric disorders associated with mutism include schizophrenia, affective disorders, conversion reactions, dissociative states, and dementias. Neurological disorders causing mutism affect the basal ganglia, frontal lobes, or the limbic system.
ObjectivesOutline the importance of setting a differential diagnosis of mutism in the Emergency Room.
MethodsReview of scientific literature based on a relevant clinical case.
ResultsMale, 58 years old. He has lived in a residence for 3 months due to voluntary refusal to ingest. Diagnosed with paranoid personality disorder. He is refered to the Emergency Service due to sudden mutism. During this day, he has been stable and suitable with a good functionality. For 3 hours he is mutist, oppositional attitude and stiff limbs, refusing to obey simple orders. Hyperalert and hyperproxia. Not staring. After ruling out organic pathology: normal blood tests, negative urine toxins and cranial CT without alterations, he was admitted to Psychiatry for observation and, finally, he was diagnosed with Psychotic Disorder NOS.
ConclusionsMutism most often occurs in association with other disturbances in behavior, thought processes, affect, or level of consciousness. The most common disorder of behavior occurring with mutism is catatonia. The differential diagnosis of mutism is complex. In some cases the diagnosis will be clarified only by careful observation and after a neurological evaluation. Published studies show neurological disorders presenting with mutism can be misdiagnosed as psychiatric.
DisclosureNo significant relationships.
Screnning of viral hepatitis in mental disorder patients: Psiqui-Clinic Programme
- M. Cavero, T. Planas, J. Goikolea, S. Lens, C. Bartrés, L. Colomer, C. García, M. Valentí, V. Ruiz, Y. Rivas, A. Benabarre, R. Catalan, G. Masana, J. Colom, X. Forns, R. Martin-Santos, Z. Mariño
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S480-S481
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The WHO would increase diagnosis and treatment of viral hepatitis in the world by 2030, based on the high efficacy of direct-acting-antivirals against HCV, extended vaccination programs in HBC, and epidemiological data. Diagnostic of HCV/HBV infection has been simplified by point-of-care (POC) devices (cheap/easy-to-use/interprete/qick-results), detecting anti-HCV-antibodies or HBV-antigen in capillary blood at the patients´site. The current seroprevalence of viral hepatitis B/C in general population in Spain is 0.5%/1% and would be higher (3-17%) in people with severe-mental-disorder due to risk factors and traditionally less access to health care.
ObjectivesTo design a screening protocol for HCV eradication and HBV-detection, and risk factors among severe-mental-disorder patients in a CommunityMentalHealthCenter. To guarantee equal access to viral hepatitis screening and therapy among this population.
MethodsOutpatients visited along one-year who accepts participate. Using POC-device for qualitative detection of anti-HCV-antibodies (Quickview-of-Lumiquick-Diagnostics®)/HBsAG (Abbott-Rapid-Diagnostics®). Socio-demographic data; mental disorder(ICD-10); HCV/HBV risk-factors; Neurotoxicity-scale (mood/cognition/sleep/gastrointestinal/sickness/motor); SF-12; Patient-satisfaction. Subjects with positive HCV/HBV POC-test will have a on-site venopuncture to assess hemograme/liver tests, and HCV-RNA (Cobas-TaqMan-RocheDiagnostics)/HBsAg-ELISA (Atellica-Siemens). In positive HCV-RNA (active infection) the psychiatric-team will inform the hepatology-team for non-invasive liver fibrosis assessment and DAA prescription. The patient will receive 8-12-weeks on-site treatment, and assessed (Neurotoxicity/SF-12).HCV cure will be confirmed by HCV-RNA in blood. Chronic-cases will be managed at Hepatology-Unit.
ResultsWe will present the results of the implementation of the programme and their ability to detect viral-hepatitis-positive cases among patients with severe-mental-disorders and to treat them effectively.
ConclusionsOur results may support the generalisation of the programme in among CMHC’s.
DisclosureNo significant relationships.
Personality disorders and Juvenil Myoclonic Epilepsy
- I. Santos Carrasco, J. Gonçalves Cerejeira, M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, G. Guerra Valera, T. Jiménez Aparicio, C. De Andrés Lobo, C. Vallecillo Adame, M. Fernández Lozano, B. Rodríguez Rodríguez, N. Navarro Barriga, M.J. Mateos Sexmero, L. Gallardo Borge
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S668
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a high comorbidity between psychiatric disorders and juvenile myoclonic epilepsy (JME), observed in up to 58% of these patients; specifically, mood disorders, anxiety and personality disorders (PD). In some patients with PD there are nonspecific alterations in the EEG, which nevertheless sometimes involve pathology. The presence of personality disorders along with JME has been repeatedly described. Previous studies have emphasized the difficulties in treating patients with JME, which have been attributed to some specific psychiatric, psychological and psychosocial characteristics.
ObjectivesDescribing distinctive personality traits in JME
MethodsReview of scientific literature based on a relevant clinical case.
Results19-year-old woman, single. Psychiatric history since she was 12 due to anxiety-depressive symptoms, after being diagnosed with JME. 4 admissions in Psychiatry, with a variety of diagnoses: eating disorder, attention deficit hyperactivity disorder and borderline personality disorder. The evolution of both disorders has been parallel, presenting epileptic seizures due to irregular therapeutic adherence together with pseudo-seizures, which made difficult their differential diagnosis. In addition, he has had frequent visits to the emergency room for suicide attempts and impulsive behaviors.
ConclusionsIn 1957, for the first time, distinctive personality traits were described in patients with JME: lack of control and perseverance, emotional instability, variable self-concept and reactive mood, which have been confirmed in subsequent studies. It is believed as epilepsy progresses, patients tend to develop symptoms of depression, anxiety, social problems, and attention deficit. Therefore, these patients have difficulty in following medical recommendations, especially precautions regarding precipitating factors for seizures.
DisclosureNo significant relationships.
Covid-19 pandemic and suicidal risk among adolescents
- J. Gonçalves Cerejeira, C. Vallecillo Adame, S. Uribe, I. Santos Carrasco, T. Jiménez Aparicio, C. De Andrés Lobo, M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, G. Guerra Valera
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S436
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The Covid-19 pandemic has had a significant impact on the mental health of adolescents. Several descriptive studies and systematic reviews have shown an increase in suicide rates in this age group.
Objectives- To present a literary review on the impact of the Covid-19 pandemic on the mental health and suicidal behavior of adolescents around the world. - To present data on admission rates due to suicidal behavior during the first year of the Covid-19 pandemic in a Spanish child-adolescent psychiatric hospitalization unit.
Methods- We will present a literature review and a retrospective cross-sectional study on admission rates for suicidal behavior in a child-adolescent psychiatric hospitalization unit. - Admission rates for suicidal behavior during the year prior to the pandemic will be compared with rates relative to the first year of the pandemic.
Results- We have found a significant increase in admission rates for suicidal behavior during the year of the pandemic. Similar results have been found in different studies and meta-analyzes. - The socio-demographic characteristics of the patients are quite similar in the two periods of time analyzed, but the reference to intra-family problems has been more frequent in the year of the pandemic.
ConclusionsOur data is in line with other studies suggesting that the Covid-19 pandemic has had a strong impact on teenage suicidal behavior.
DisclosureNo significant relationships.